What is the Cornea?
The cornea is the clear front of the eye that covers the colored iris and the round pupil. Light is focused while passing through the cornea, so we can see. To stay clear the cornea must be healthy.
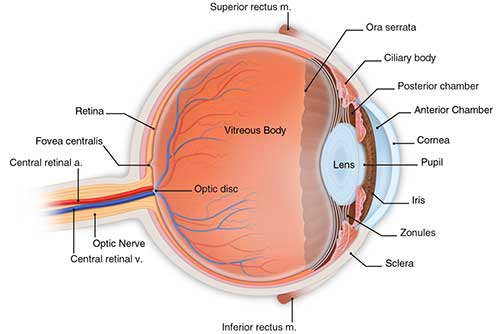
Corneal Infections & Diseases
The cornea can be damaged by trauma or injury. At other times, bacteria or fungi from a contaminated contact lens can pass into the cornea. Situations like these can cause painful inflammation and corneal infections called keratitis. These infections can reduce visual clarity, produce corneal discharges, and perhaps erode the cornea.
Corneal infections can lead to corneal scarring, which can impair vision and may require a corneal transplant. A hereditary condition called Fuchs’ dystrophy, and Keratoconus, a thinning of the cornea, are examples of other conditions that can cause corneal failure.
A corneal transplant is needed when the clarity of the cornea is such that vision cannot be corrected with eyeglasses or contact lenses, or if painful swelling cannot be relieved by medications or special contact lenses.
Corneal Transplants
Until the last few years, full-thickness corneal transplantation was the procedure performed to treat most disorders affecting corneal clarity. The drawbacks of induced astigmatism, unpredictable refractive changes, weakening of the eye, and risk of graft rejection prompted the development of faster, safer, and better solutions. The disorder of corneal clarity caused by disorders of the endothelium can be cured by the replacement of that layer as opposed to the entire cornea.
A procedure known as Descemet’s Stripping Automated Endothelial Keratoplasty (DSEK) revolutionized corneal transplantation. In this operation, the abnormal endothelial layer is removed and replaced by a thin disc of donor endothelium placed inside the eye through a small peripheral incision.
The tissue adheres to the back of the cornea because of the natural suction applied by the healthy endothelium. The improvement in corneal clarity begins immediately, and patients often are able to get new glasses one month after surgery.
The risk of graft rejection is halved in comparison with full-thickness transplantation, and the possibility of globe rupture is significantly reduced. For many with corneal clouding, DSEK offers more predictable visual outcomes.
DMEK
Over the last decade, a lot of progress has been made in the successful outcomes of corneal transplants. The latest is a new procedure known as Descemet’s Membrane Endothelial Keratoplasty (DMEK). DMEK further improves this procedure by using a thinner disc of tissue made up of only endothelium and Descemet’s membrane.
This tissue is more difficult to handle, but once in place provides improved visual outcomes, as well as, decreased rejection rates compared to both DSEK and full-thickness corneal transplants. DMEK may be a better option for patients with Fuch’s Dystrophy and no other serious ocular problems.




