The cornea is the clear, protective outer layer of the eye. Along with the sclera (white of the eye), it serves as a barrier against dirt, germs, and other particles that can harm the eye’s delicate components. The cornea also filters out some of the sun’s ultraviolet light.
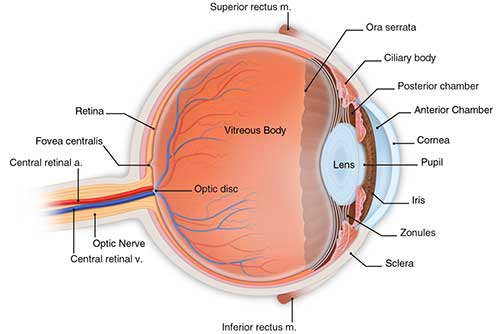
The cornea plays a key role in vision too. As light enters the eye, it is refracted, or bent, by the outside shape of the cornea. The curvature of this outer layer helps determine how well your eye can focus on objects close-up and far away.
There are three main layers of the cornea:
- Epithelium: The most superficial layer of the cornea, the epithelium stops the outside matter from entering the eye. This layer of the cornea also absorbs oxygen and nutrients from tears.
- Stroma: The stroma is the largest layer of the cornea and is found behind the epithelium. It is made up mostly of water and proteins that give it an elastic but solid form.
- Endothelium: The endothelium is a single layer of cells located between the stroma and the aqueous humor – the clear fluid found in the front and rear chambers of the eye. The endothelium works as a pump, expelling excess water as it is absorbed into the stroma. Without this specialized function, the stroma could become waterlogged, hazy and opaque in appearance, also reducing vision.
The term “corneal disease” refers to a variety of conditions that affect mainly the cornea. These include infections, degenerations, and many other disorders of the cornea that may arise mostly as a result of heredity.
What Are Symptoms When Something is Wrong With the Cornea?
With its ability for a quick repair, the cornea usually heals after most injuries or disease. However, when there is a deep injury to the cornea, the healing process may be prolonged, possibly resulting in a variety of symptoms, including:
- Pain
- Blurred vision
- Tearing
- Redness
- Extreme sensitivity to light
- Corneal scarring
If you experience any of these symptoms around your cornea, seek care from an eye doctor. They may indicate a more serious problem or require special treatment.
What Conditions Can Damage the Cornea?
Keratitis
This is an inflammation of the cornea that sometimes occurs with infection after bacteria or fungi enter the cornea. These microorganisms can enter the eye after deep injury, causing infection, inflammation, and ulceration of the cornea. Though uncommon, this type of infection can also arise after an injury from wearing contact lenses.
Symptoms of keratitis include:
- Severe pain
- Reduced visual clarity
- Corneal discharge
Treatment usually includes antibiotics or antifungal eye drops.
Ocular Herpes (Herpes of the Eye)
This is a viral infection of the eye that may reoccur. The main cause of ocular herpes is the herpes simplex virus I (HSV I), the same virus that causes cold sores, but it can also result from the sexually transmitted herpes simplex II virus (HSV II) that causes genital herpes.
Ocular herpes produces sores on the surface of the cornea and, in time, the inflammation can spread deeper into the cornea and eye.
There is no cure for ocular herpes, but it can often be controlled with the use of antiviral drugs.
Herpes Zoster (Shingles)
Shingles is a recurrence of the chickenpox virus in people who have already had the disease. After having chickenpox, this virus usually remains inactive within the nerves of the body. It can later travel down these nerves, infecting specific parts of the body, like the eye. Herpes zoster can cause blisters or lesions on the cornea, fever, and pain from nerve fibers. Corneal lesions usually heal by themselves, but antiviral treatment may reduce the inflammation.
Shingles can occur in anyone exposed to the chickenpox virus, but there is an increased risk in:
- Older adults, especially over age 80
- People with a weakened immune system
For those over 50, there is now a vaccine that can reduce the risk of getting shingles. See your doctor if you have any symptoms of shingles.
Corneal Dystrophies
There are over 20 corneal dystrophies, diseases that cause structural problems with the cornea. Some of the most common are:
Keratoconus
Keratoconus is a progressive, noninflamatory, eye condition where the cornea thins and weakens, causing the typically round dome shape to bulge and become cone shaped. Sometimes occurring as early as adolescence, this disease changes the curvature of the cornea, creating either mild or severe distortion, called astigmatism, and usually nearsightedness. Keratoconus may also cause swelling and scarring of the cornea and vision loss.
Things associated with keratoconus include:
- Genetics (a person can inherit a tendency to get the condition from a parent.)
- Eye trauma (for example, from rubbing your eyes or long-term use of hard contacts)
- Eye diseases, such as retinitis pigmentosa, retinopathy of prematurity, vernal keratoconjunctivitis
- Other diseases, like Down Syndrome, osteogenesis imperfecta, Addison’s disease, Leber’s congenital amaurosis, and Ehlers-Danlos Syndrome
At first, the condition is correctable with glasses or soft contact lenses. But, as the disease progresses, you may need to wear rigid gas permeable contact lenses. Corneal cross-linking, Intacs, and corneal transplantation may also be necessary.
Our fellowship trained cornea specialists are offering, iLink™ corneal cross linking, the only FDA-approved procedure for the treatment of progressive keratoconus, proven safe and effective in rigorous clinical studies. This minimally invasive outpatient procedure uses specially formulated prescription eye drops called Photrexa® (riboflavin 5′-phosphate ophthalmic solution) and Photrexa® Viscous (riboflavin 5′-phosphate in 20% dextran opthalmic solution), combined with ultraviolet (UV) light from the KXL System, to slow or halt the progression of the disease. This office procedure takes about 2 hours and is widely covered by commercial insurance policies. Please contact your carrier to understand your responsibilities. If you have been diagnosed with progressive keratoconus, ask your doctor if you might be an appropriate candidate for the iLink procedure.
Summary of Information About Corneal Cross-Linking
What is corneal cross-linking?
• iLink™ is the only FDA-approved corneal cross-linking procedure for the treatment of progressive keratoconus. This minimally invasive outpatient procedure uses specially formulated prescription eye drops called Photrexa® and Photrexa® Viscous, combined with uv light from the KXL System to slow or halt the progression of disease.
• The safety and effectiveness of corneal cross-linking has not been established in pregnant women, women who are breastfeeding, patients who are younger than 14 years of age and patients 65 years of age or older.
What warnings should I know about iLink™ corneal cross-linking?
• Ulcerative keratitis, a potentially serious eye infection, can occur
• Your doctor should monitor your resolution of epithelial defects if they occur
What are the side effects of iLink™ corneal cross-linking?
• The most common ocular adverse reactions in any corneal cross-linked eye were haze (corneal opacity), inflammation (punctate keratitis), fine white lines (corneal striae), disruption of surface cells (corneal epithelium defect), eye pain, reduced sharpness of vision (visual acuity) and blurred vision.
The risk information provided here is not comprehensive. To learn more, talk about iLink™ corneal cross-linking with your healthcare provider.
The FDA-approved product labeling can be found at www.LivingWithKeratoconus.com. You are encouraged to report negative side effect of prescription drugs to the FDA. Visit FDA.gov/medwatch or call 1-800-FDA-1088.
Map-Dot-Fingerprint Dystrophy
Map-dot-fingerprint dystrophy is the abnormal appearance of the basement membrane of the epithelium of the cornea. As this membrane that separates the epithelium and stroma grows irregularly (thicker in some places, thinner in others), findings in the cornea appear, resembling maps, dots, and small fingerprints.
Map-dot-fingerprint dystrophy usually affects adults between the ages of 40 and 70, or children as a result of heredity. It is usually painless and causes no vision loss, and sometimes clears up without treatment. In some cases, however, epithelial erosion may occur. Epithelial erosion can expose the nerves lining the cornea, causing severe pain. The cornea’s normal curvature may be altered causing astigmatism and nearsightedness.
As the cornea is altered, vision may be blurry and accompanied by:
- Moderate to severe pain
- Increase sensitivity to light
- Excessive tearing
- A feeling that something is in your eye
Treatment may include an eye patch, eye drops, and ointments.
Fuchs’ Dystrophy
Fuchs’ dystrophy is the gradual deterioration of endothelial cells for no apparent reason. As these cells thin over time, the cornea is less capable of removing water from the stroma, causing it to swell and distort vision. Haze and small blisters on the corneal surface may also appear.
As a slowly progressing disease, signs of Fuchs’ dystrophy begin to appear in people 30 to 40 years of age, but it doesn’t normally affect vision until about 20 years later. It is more common in women than in men.
An early sign of Fuchs’ dystrophy includes awakening with blurred vision that gradually clears up during the day. As the disease worsens, swelling becomes more consistent and vision blurs.
Treatment includes:
- Ointments
- Soft contact lenses
- Drying of blisters with a hairdryer two or three times per day
- Corneal transplant
Lattice Dystrophy
Lattice dystrophy is characterized by the presence of abnormal protein fibers throughout the stroma. Although this condition can occur at any age, early changes can be seen in childhood.
Lattice dystrophy gets its name from the clear overlapping lines of proteins in the stroma. This can make the cornea cloudy and reduce vision. In some people, these proteins may cause epithelial erosion.
Treatment of Lattice dystrophy includes:
- Prescription eye drops
- Ointments
- An eye patch
- Corneal transplant
Symptoms may disappear with treatment, but a corneal transplant may be required. Although the results of this surgery are very good, lattice dystrophy may reappear in transplant patients.




